Academic Research
My research into positron emission tomography (PET) was conducted between September 1999 and October 2001 and resulted in the award of the degree of Doctor of Medicine by the University of London in June 2003.
PET is a functional imaging modality that is able to detect cancer cells based on the abnormal metabolism of certain organic chemicals within the cell. My interest in PET was cultivated by the knowledge that cancer cells metabolise glucose in a different way to normal healthy cells. If one injects a cancer patient with picomolar concentrations of fluorine-18 labelled glucose, a radiotracer known as FDG, the substance accumulates in the cancer cells at higher concentrations than normal cells. Using highly sophisticated detection scanners one can acquire a detailed image of where the tumour is in any one of the transaxial, sagittal or coronal planes (figure below). In fact, this data set can be re-processed on a computer workstation into a three dimensional image.
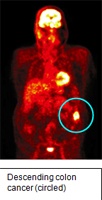
Because the cellular changes that are detected by PET precede the structural changes that are related to cancer transformation and detected by conventional imaging modalities such as CT and MRI, there is a potential to detect tumours at an earlier stage. My thesis examined the role of FDG PET imaging in cancer imaging using colorectal cancer as a model. At the time of the project I worked in one of the only units in the UK with a full ring multicrystal state of the art PET scanner and the research group was the only unit publishing substantial data on this subject in the UK. This machine has recently been upgraded to a combined PET/CT scanner of which there are only about 40 in the world. The data acquired from my research has been presented to a number of learned societies and been published as original papers, book chapters and in various electronic media.
The work evolved further as we studied a new radiotracer, FLT, previously unused in the UK. I was awarded a grant of £30,000 to initiate this work. During the research period I have submitted numerous grant applications as well as research ethics applications. In addition, because the work involved radioactive material applications had to be made to the appropriate authorities. I also have experience in cell culture techniques and autoradiography while working with endothelin-1, an angiogenic growth factor for colorectal cells in vitro.
The results of my work have been encouraging and although at first glance the technique appears a remote esoteric subject, PET is now part of the mainstream of imaging modalities in surgical oncology both in Europe and North America. The situation in the UK has mirrored these developments. I have personally benefited from my time in research through the self discipline needed to organise and see the work through, acquiring a questioning approach to published data and translating this approach to my daily surgical activities. I am supervising research myself and have continued both clinical and laboratory research at Colchester General Hospital and the University of Essex. I have accepted the responsibility of supervising the projects of students conducting research towards MD's at the University of Essex and have been nominated to the post of Honorary Senior Lecturer. In recognition of this work I have been awarded a research grant by the Royal College of Surgeons of England. I carry out teaching and supervision of postgraduate nursing students in advanced prescribing as well as those taking the Advanced Theatre Practitioner Diploma.
I have continued my portfolio of personal research in collaboration with colleagues in the Surgical Department as well as Dr. Bruce Sizer in the Department of Oncology. Current clinical projects include investigation into training in advanced laparoscopic surgery, the timing and efficacy of laparoscopic surgery for patients suffering from locally advanced rectal cancer who have received long course chemoradiotherapy and laparoscopic colorectal surgery.
